Holistic Mental Health Defined
According to the World Health Organization
and the National Institute of Mental Health, “access to the social determinants of health are far more important to mental health than access to health care alone“. These social determinants include:
- Affordable housing,
- Reasonable access to educational opportunities
- Reasonable access to job opportunities
- Community inclusion — a feeling of acceptance within a larger peer group or community.
As crucial as quality mental health care is to recovery and daily management of symptoms, without these in place. what is otherwise high-quality mental health care will only go so far.
“We who struggle with these disorders can lead full, happy, productive lives if we have the right resources.” So said Elyn Saks, schizophrenia survivor, author, mental health advocate, MacArthur Fellow, and Law Professor at the USC Gould School of Law.
First, there is the social stigma.
Battling a mental illness is a challenge in itself. Then there is added social stigma, which in Psychology Today was defined as “characterized by prejudicial attitudes and discriminating behavior directed towards individuals with mental health problems as a result of the psychiatric label they have been given.
Then there is self-stigma
This is the most dangerous force in a person’s mental health recovery.
“Self-stigma causes the sufferer to consciously or subconsciously perceive themselves, or their illness in the prejudiced way society does.” This leads to loss of self-confidence, low-self esteem, poor self-efficacy, and self-isolation.
~Why Self-Stigma is the Most Dangerous Pitfall when Battling Mental Illness
Worst of all, it prevents the sufferer from seeking treatment or reaching out to others. It is not all too different (not to use an extreme example) in some ways to forced solitary confinement in prisons. In this case, it is self-imposed. It is common knowledge that extended social isolation can deteriorate a person’s mental health, even among those who do not have a diagnosis of mental illness.
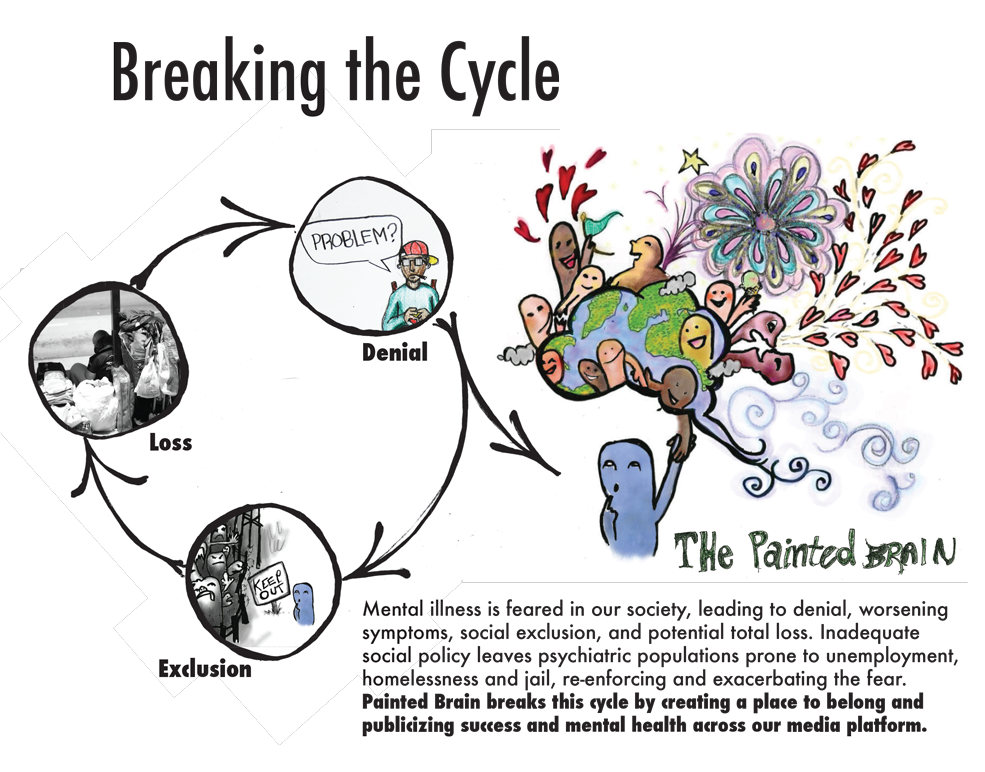
The Vicious Cycle – Denial, Isolation, Loss
Too often, psychiatric hospitals, inpatient or outpatient clinics, assisted-living facilities, and many, many treatment centers meant to address problems like depression and suicide fail to take into account the wider, social forces affecting a person’s mental health. Isolation is one of them.
Isolation is often a result of the brutal combination that comes out of the very distressing nature of mental illness itself with the added “lash” of self-stigma.
Isolation is the most pressing issue in young adults’ mental health.
People with mental illness have a harder time finding good jobs or safe housing. People with mental health conditions face an 80% unemployment rate. Out of almost 1500 respondents to one survey, HALF of them stated they would not socialize, work with, or have a family member marry someone with a mental illness.
A person who has just been discharged from a psychiatric hospital or released from the streets or jail needs more than a roof over their head. Meaningful activities, meaningful inclusion, and acceptance within a peer group or community, decent opportunities to get education and training; these are every bit as important as quality health care; and too often absent. Absent a path to reintegration, relapses become too common.
Self-stigma, social stigma, and isolation become a vicious cycle.
Meanwhile, the chances of jail recidivism, repeat hospitalizations, suicides, and the economic plus human toll of depression (on the individual and their families) only continues to mount, not decrease. Despite the rising numbers of people taking antidepressants and more attention given to mental health prevention, the core problem remains unsolved.
“Mental Illness is a Social Problem.
Art Brings People Together.
Change Begins with Simple Ideas.”
~Dave Leon, Founder and Executive Director, Painted Brain
The idea of infusing art, skills training, and peer-led art projects into mental health is for many in the mental health care profession, new unchartered territory, and that is about to change.
In fact, it is already changing. Art serves as an excellent addition, a compliment, to standard treatment programs. Art is being increasingly recognized (through academic studies and healthcare institutions) as a universal form of expression that can heal. Art is also a catalyst that brings people together, and art is a glue that builds community.